Our stories
Latest | Home | About | Our People | Bridging Our Divide | CLAFH | Events| News | Affiliates | Training
Research
Practice
Policy
Improving health through nursing innovation and leadership
The Institute for Policy Solutions at the Johns Hopkins School of Nursing


Dr. Vincent Guilamo-Ramos believes in equitable, whole-person care for all Americans. As a nurse, researcher and advocate, Dr. Ramos knows this can happen through nursing’s capacity as expert clinicians, paired with the power of policy. His role as the new executive director of the Institute for Policy Solutions at the Johns Hopkins School of Nursing aims to drive this vision.


Johns Hopkins School of Nursing Rising Professor Dr. Kamila Alexander and her colleague Dr. Tiara Willie joined fellow advocates and policy makers to offer evidence-based policy solutions and support for victims, survivors, and families of murdered or missing Black women and girls. Their work examines and brings to light this underreported issue which is often uncoordinated across state lines.




Nurse Lisa Stambolis is leading the charge to better the health outcomes in low-income areas of Baltimore. In collaboration with the schools of nursing at University of Maryland, Morgan State and Coppin State, the Neighborhood Nursing model has the potential to improve many crucial health indicators by focusing on prevention, amplifying wellness, and learning what matters most to people, all in the comfort of their homes and neighborhoods.


DNP/PhD student Erika Estrada-Ibarra works alongside her advisors Drs. Eliana Perrin and Lucine Francis at the nurse-led Center for Community Programs, Innovation, & Scholarship (COMPASS) to bring health education and resources to low-income, underinsured and noninsured populations in Maryland. Her work in Baltimore provides support for her research to implement early nutrition education and identify barriers to reduce pediatric obesity while improving lifestyle in the most overweight and obese regions in the country.




When Dr. Laura Samuel talks about food insecurity, she often draws upon her own experiences spending part of her youth in a mobile home in coastal Maine, one of six children in a hardworking family that often faced tough choices regarding money. Today as a nurse and assistant professor at the Johns Hopkins School of Nursing, her research focuses on economic and racial disparities and their effects on public health, aging, disabilities, and chronic care, including food insecurity.


Thousands of patients across the State of Maryland have been tested and, as necessary, linked to care for HIV and other infectious illnesses. Led by Dr. Jason Farley, the Center for Infectious Disease and Nursing Innovation (CIDNI) collaborates closely with the Baltimore City Department of Health and the Maryland Department of Health along with many federally qualified health centers. His research in Baltimore intersects with is research in South Africa to provide care for thousands more.




Dr. Sarah Szanton co-developed the visionary CAPABLE program after years spent providing house calls predominately to low-income, African-American older adults in West Baltimore. Now in 21 states and internationally in Australia and Canada, the program has been proven to lower health care costs. Roughly $3,000 in program costs saves $22,000 per person in avoided medical costs and nursing home admissions.


As a first-generation immigrant from Costa Rica and 3rd year PhD Candidate, Laura Mata Lopez’s research is informed by her lived, clinical, advocacy, and policy experiences. In her research, she engages community and stakeholders as partners to identify key cultural, communal, and structural factors – such as immigration and health policies – that can mitigate (or exacerbate) the risk of suicide among Latina immigrants in Baltimore.


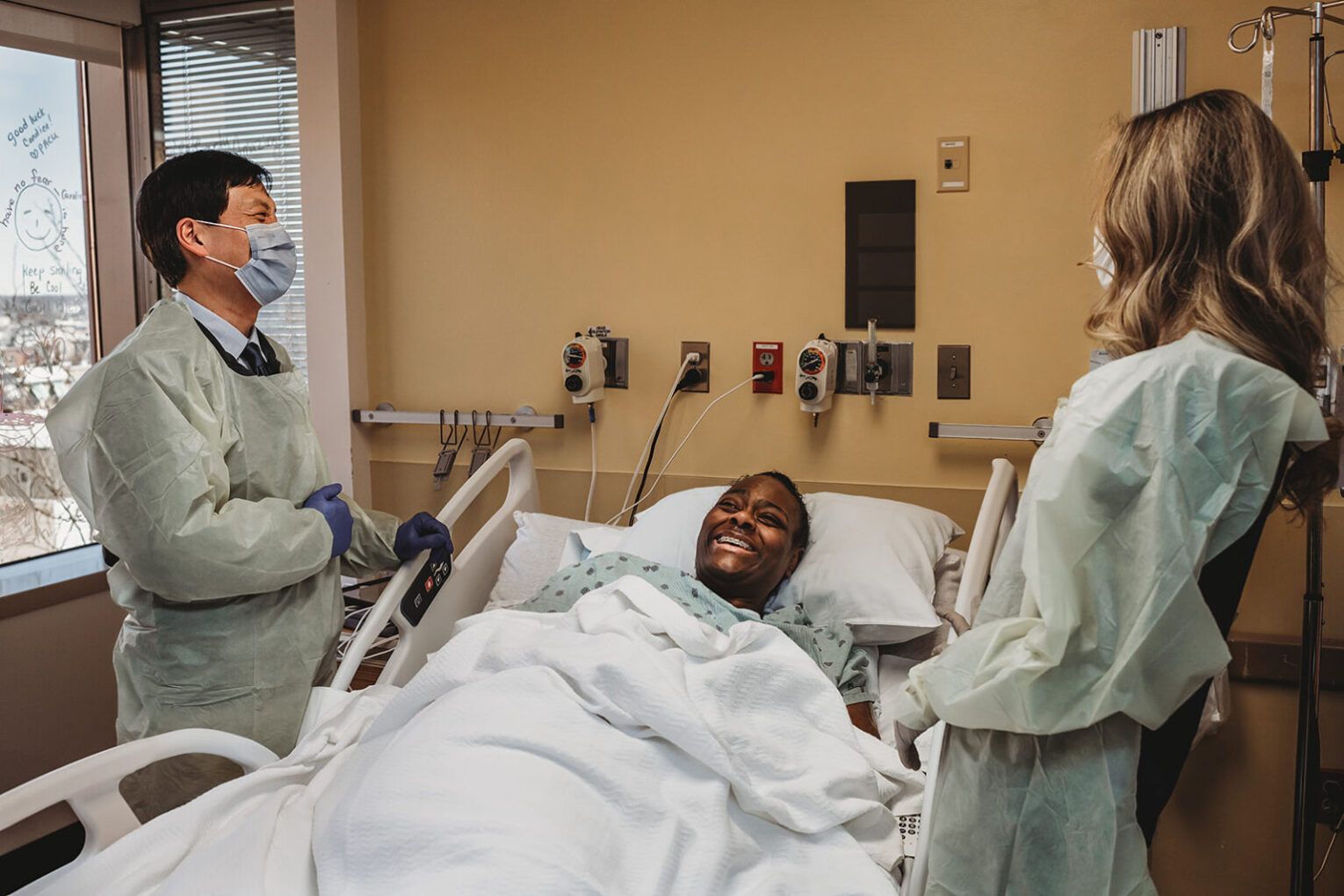

PICAR, the Palliative Interprofessional Collaborative for Action Research, was founded by Dr. Rebecca Wright from the Johns Hopkins School of Nursing along with Drs. David S. Wu and Danetta Sloan from the Schools of Medicine and Public Health, respectively. The initiative provides an ‘action research’ approach enabling the team to conduct research, in real time, that responds to clinical challenges facing the Palliative Care Program at the Johns Hopkins Bayview Medical Center.


