For those of you who have been following my blog, well, first and foremost … let me say Wow! Thanks for reading! 😀 I appreciate it very much. Secondly, I wanted to remind you of the blog entry I posted around Jan 2012 about an experience I had over winter break while watching a wound cleaning and how I threw up and almost passed out. Post-incident, I was able to laugh at myself and I filed the situation into the back of my mental bank of memories/experiences to remember some time in the far away distant future. Well … that “far away distant future” was really not as far away as I had hoped it would be.
Today during clinicals I watched a patient get his tracheotomy tube removed. Pretty benign, right? That’s what I was thinking! Well, Caitanya–think again. I’m not sure when the tides turned but suddenly, that feeling of queasiness in the stomach, the cold/hot tingling in my body, objects in my vision becoming a tad too sparkly creeped up on me. I was very aware of the change in my body and forced myself to breathe deeply. I thought, “The patient is okay, you’re okay, stay calm.” I concentrated on “Bad feeling in stomach, be gone!” However, unfortunately, that self-coaching didn’t help and I quickly sat down in a chair away from the bed. My head was throbbing, I felt like I could have thrown up–all sensations familiar from the last time.
However, this time my feelings are different from the last time. I admit I feel some shame over this experience, especially since it is no longer the first time that something like this has happened.
So I ask myself: What to do? I did some searching online and apparently, this is not an isolated incident, that plenty of nursing students–as well as medical students–have either almost fainted or totally fainted while watching something that did not agree with them.
Does this make me feel better? I guess so. However, my ego is screaming, “You wimp! It was just a hole in someone’s trachea! It’s not like his brains were spilling out all over the place!” If only my body could listen and understand this “logic.”
I wonder what this means for me. Am I really cut out for this nursing thing? My clinical instructor said maybe this means I need to work in an outpatient setting. Ultimately, that is what I’d prefer to be doing, but I’d still like to be able to stomach looking at open wounds because I’m sure someone will come in one day with some mean and nasty looking orifice that should not be where it is.
Anyhow, I am not close to admitting “defeat” (it’s not really defeat, this is just me being silly). My goal: Desensitize myself by the end of the semester, if not at least by the end of the school year. And how do I plan on going about this? Brilliant idea, Caitanya: We had a burn unit nurse come and speak to our class earlier this week and she offered us to come for some share time. If there’s one thing I cannot stand even in thought is a burn victim. I felt nauseous all during the lecture just looking at the pictures. But sometimes immersion is the way to do it! I am writing to this nurse, requesting for share time on the burn unit. I figure, if I can remain standing in the burn unit for longer than 3 minutes, then I’ve conquered this!
Is it weird that I’m running straight into the fire? Perhaps. However, I would like to take the bull by the horns and overcome this issue of mine (yes, it has become an issue).
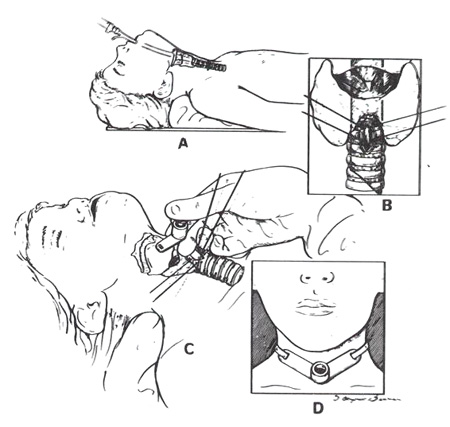
Okay, everyone. I can do this, for sure! It is doable. And if anyone has any special tips, I welcome them 🙂 (BTW, I know the picture of the trach above is not of a removal, but I thought it was a good visual example for those who don’t really know what one is)
(Update: Burn nurse kindly dissuaded me from doing share time on the burn unit. Onward we go …)