As Applications Surge, Need for Greater Capacity Grows
Global Research That Changes Lives
Faculty News
The Final Word on Breastfeeding
Global Connections
Toward a Better Response to Domestic Violence
SimMan, the Lifelike Addendum
Milestones
Asking Questions to Improve Safety
Magnets to Excellence
As Applications Surge, Need for Greater Capacity Grows

Applications to the School of Nursing’s baccalaureate program are up 21 percent, from 2002-2003 to 2003-2004, according to Sandra Angell, associate dean for student affairs. Add that to last year’s increase and that’s a lot of activity in the School of Nursing.
The spike in applications is good news during today’s nursing shortage—a shortage that is only expected to get worse. The Bureau of Labor Statistics is projecting more than one million vacant RN positions by 2010.
The bad news—or at least the problem—is accepting these much needed applicants. The American Association of Colleges of Nursing reports that baccalaureate enrollment nationwide went up 16.6 percent from 2002 to 2003. That’s a healthy increase but not nearly enough: An article in the November/December 2003 issue of Health Affairs predicted that enrollment needs to increase at least 40 percent annually just to replace retiring nurses.
At the Hopkins University School of Nursing, enrollment went up 8 percent from 2002 to 2003 in the baccalaureate program. A similar increase is expected in 2004. The deterrent to larger increases is universal: capacity.
“If we had the space and more faculty, we could take more students,” says Mary O’Rourke, director of admissions and student services. “Last year, we had a waiting list. I didn’t move one student off that list.” The increase in applications also means that even more would-be nurses will be turned away.
Preliminary plans and a fundraising campaign are in the works to put an addition on the building that would expand capacity by 20 to 25 percent, according to Dean Martha N. Hill, PhD, RN, FAAN. That’s five or six years away. In the meantime, to accommodate more students, some courses have been sectioned. Others have been simulcast.
Not that anybody is grumbling about the surge in applications. “We’re thrilled to see the increased interest in nursing as a profession,” says Hill, who remembers when people thought of nursing as manual labor. She recalls the time a Dickinson College advisor brought a busload of students to the school. “They had no idea what nursing was or how rigorous the curriculum was. One of them said, ‘I thought it was all about bed pans, and who wants to do that?’”
Thanks in part to the spotlight the nursing shortage has shone on the profession, the public is realizing that nursing is an intellectually challenging career. Public perception no doubt has been swayed by factors such as Johnson & Johnson’s recent nationwide marketing campaign in support of the nursing profession, and new studies demonstrating the very real effect that nurses have on patient survival.
Moreover, salaries are up and working conditions and benefits are improving as understaffed hospitals try to attract nurses. The tight economy doesn’t hurt, either. “Nursing applications often rise when unemployment is high,” says Linda Pugh, PhD, RNC, FAAN, associate professor and director, baccalaureate programs. “And I always think that with a bachelor’s in nursing, the world is your oyster.”
— Kristi Birch
Global Research That Changes Lives
This summer, thanks to an extended grant from the Fogarty International Center of the National Institutes of Health, eight Johns Hopkins students will join the Minority Investigator Research Training (MIRT)-Global Health Promotion Research Program and travel to four continents to conduct research on health topics as common and diverse as diabetes, pain, and domestic violence. Six of these students are from the School of Nursing; one is from the Bloomberg School of Public Health; and the other is from the Krieger School of Arts & Sciences. Five other students—from Brown, Columbia, Winston-Salem State, North Carolina A&T State, and Cornell universities—will also participate in the program.
Now in its fifth year, the program was created by the school’s Fannie Gaston-Johansson, DrMedSc, RN, FAAN, director of international programs, to address neglected global health issues, especially those disproportionately affecting under-served populations. Over the summer, students work with Johns Hopkins faculty and faculty at research institutions in other countries. “They grow, they experience, and they are different people when they come back,” says Gaston-Johansson, the school’s Elsie M. Lawler Research Chair. “They have much more definite plans about their future.” The program this year saw a 50 percent increase in applications over last year.
The School of Nursing participants are Sally Huynh, Uruaku Obasi, Hyunjeong Park, Gina Pistulka, Mitra Rangarajan, and Shiree Southerland.
Park thinks that the cardiovascular research she will be doing at the Korean Institute for Health and Social Affairs will relate to the research in hypertension she conducts as a research assistant at the School of Nursing. Pistulka will also be in South Korea, where she will do research on chronic diseases that will inform her dissertation as well as the community-based interventions she hopes to do in the future.
When she was earning a doctorate in community health, Southerland studied the relationship between condom usage and HIV/AIDS among African American females. Now she will be at the University of Natal in South Africa, doing research in HIV/AIDS and adolescent health. Rangarajan worked as a nutritionist and diabetes educator before entering nursing school. This summer, she will be at the University of Newcastle in Australia studying the relationship of stress to metabolic syndrome, a group of health risks that can increase the chance of diabetes and heart disease.
What makes this experience unique for the School of Nursing students is the chance to see how research is conducted in another country—and from a nursing perspective, participants say.
“I’ve done research in other places but not as a nurse,” says Huynh, who will study the biology of stress with researchers at the University of Newcastle. “I saw the program in Australia and I thought, how will it be in another country? What can I learn there and what can I teach them?”
Obasi will be at the Medical Research Council in Durban, South Africa, studying domestic violence. “I wanted to get a broader view of nursing,” she says. “There is so much we can get from this one experience.”
— KB
Faculty News
Patricia Abbott, PhD, RN, FAAN, was elected to the American College of Medical Informatics.
Kay Cresci, PhD, RN, CCRN, was inducted as a fellow of the National Gerontological Nurses Association.
Marion D’Lugoff, MA, RN-CS, has been granted a 2004 Healthy Vision 2010 Community Award from the National Institutes of Health National Eye Institute. The funds will be used by the Wald Community Nursing Center to promote healthy vision in East Baltimore.
Cheryl Dennison, PhD, RN, CRNP, received the 2003 Best Abstract Award from the American Heart Association’s Council on Cardiovascular Nursing for her research abstract titled “Comprehensive Hypertension Care in Underserved Urban Black Men: High Follow-Up Rates and Blood Pressure Improvement over 60 Months.” Other authors who worked on the abstract are Martha N. Hill, Lee R. Bone, and David M. Levine.
Sue Donaldson, PhD, RN, FAAN, served as a panel member on the National Institutes of Health Consensus Development Conference on Total Knee Replacement.
Lori Edwards, MPH, RN, APN, BC, received the “Julie Center’s Best” award from the Julie Community Center.
Robert Feroli, PharmD, adjunct associate professor, received the W. Arthur Purdum award from the Maryland Society of Health-System Pharmacists.
Miyong Kim, PhD, RN, was elected a fellow of the American Heart Association and the Council on Cardiovascular Nursing.
June Miller, PhD, RN, was elected president of the Transcultural Nursing Society.
Rosemary Mortimer, MSEd, MSN, RN, received the Centennial Award for Outstanding Mentoring from the Maryland Nurses Association.
Sharon Olsen, MS, CS, NP, AOCN, co-edited a book titled Instruments for Clinical Health-Care Research, published recently by Jones and Bartlett Publishers. Contributors from the School of Nursing included faculty members Hae-Ra Han, Miyong Kim, Linda Pugh, Peggy Soderstrom, and former faculty member Patricia Grimm.
Cynda Rushton, DNSc, RN, FAAN, chaired the 19th annual Pediatric Nursing Conference. Approximately 260 nurses attended sessions on topics ranging from caring for children with chronic illnesses to minimizing legal liability. Rushton has chaired the conference for 15 years.
Janet Selway, DNSc, CRNP, was elected to the American College of Nurse Practitioners (ACNP) Board of Directors as a State Affiliate representative for a two-year term.
Phyllis Sharps, PhD, RN, FAAN, has been selected as a member of the Research Committee of the National Black Nurses Association.
Dan Sheridan, PhD, RN, received the 2003 Medical Award from the Maryland Network Against Domestic Violence.
Jo Walrath, PhD, RN, was appointed to the editorial board of The Journal of Nursing Care Quality.
The Final Word on Breastfeeding
In 107 pages bound with a pink cover, Linda Pugh, PhD, RNC, and a volunteer team of nursing students have written the book on breastfeeding resources in Maryland. The comprehensive manual, Maryland Breastfeeding Resource Handbook (Second Edition), was issued last spring, and, according to Pugh, has received “very positive feedback” from Maryland’s pediatric community.
Pugh, an associate professor and director of the baccalaureate program at the School of Nursing, is well-known for her research involving breastfeeding promotion among low-income mothers. She is currently the principal investigator of a four-year, $2 million study to assess the cost-effectiveness and success of encouraging low-income mothers, through educational intervention and peer support, to breastfeed their newborns for a minimum of six months.
The handbook, the only one of its kind for Maryland, provides a comprehensive index on a range of topical resources around the state, including breastfeeding support groups, agencies, classes, equipment companies, and additional information in the form of magazines, books, videos, and Web sites. The handbook is being distributed to pediatricians and nurse practitioners in community health practices, as well as to offices of the federally sponsored Special Supplemental Nutrition Program for Women, Infants, and Children.
“It’s a wonderful resource and a real practice enhancement for anyone who works with mothers and babies,” says Pugh.
The handbook was printed and distributed free of charge by the Maryland Department of Health and Mental Hygiene’s Family Health Administration Center for Maternal and Child Health, in collaboration with the Maryland Breastfeeding Promotion Task Force.
The handbook is a result of an all-volunteer effort, notes Pugh, thanks to the work of former students (now graduates) Marcy Nelson, Lee Ann Walker-Illig, Sarah Howard, and Rosalyn Hamilton.
— Dave Beaudouin
Global Connections
From Brazil to Baltimore and Back
Sayonara Barbosa holds the distinction of being the first and only nurse from Brazil to receive a grant from the Fulbright Visiting Scholars Program. Barbosa, a critical care nursing assistant professor at Federal University of Santa Catarina and a doctoral student at Federal University of Sao Paola, will spend six months at the School of Nursing studying nursing informatics. During her stay, which began in February, she is developing and implementing a Web-based simulation in critical care nursing. When she returns to Brazil, she will evaluate it as a complementary teaching tool in her undergraduate nursing course.
While here at Hopkins, Barbosa will also obtain a broader view of nursing informatics education and training in the United States through observation, laboratory, collaborative, and lecture experiences.
“For us in Brazil, it is very difficult to be a Fulbrighter,” says Barbosa. “I was really surprised and proud to receive the grant. Best of all is to be recognized as a researcher with demonstrated leadership potential, and to have the opportunity to learn more about the U.S. culture and share knowledge about the Brazilian culture.”
—Ming Tai
Beijing for the Holidays
While other nursing students were headed home for the winter holidays, doctoral student Jason Farley traveled halfway around the world.
Participating in Hopkins’ first international infection control internship, Farley, a Hopkins Hospital adult nurse practitioner, infection control consultant, and member of the hospital’s SARS task force, spent three weeks at the Beijing United Family Hospital in China. In that short time, he worked with the administrators and staff of the 50-bed hospital to develop an infection control strategic plan.
Farley first explored current patient care practices, asking individual department heads to identify problem areas related to infection control. “I couldn’t have gone into the hospital and said, This is wrong, That is wrong,” he explains. “So I presented evidence-based guidelines and then asked them what needed to be corrected and changed. It was an interactive process.” Farley found the staff very motivated, and changes were often made on the spot. “The resilience of the staff was amazing,” he says.
During his stay, Farley visited surrounding hospitals and observed how SARS has impacted the Chinese health care system’s focus toward infection control efforts. He has been invited to come back for a second visit this summer.
—MT
Toward a Better Response to Domestic Violence
On a hot morning last August, a car pulled up to the Johns Hopkins Hospital. The driver, a well-dressed man in his mid-30s, dropped off his wife at the curb and entered the parking garage. Sporting a bruised arm and black eye, the woman entered the emergency room in a daze, where she remained unescorted for only a brief moment before she was quickly joined by her husband. A controlling presence, he told the triage nurse the story of how his wife, being clumsy once again, fell down the stairs.
The incident on this particular day was staged; the husband and wife were actors. But unfortunately, such a scene is not uncommon, according to Jacquelyn Campbell, PhD, RN, FAAN, professor, associate dean for faculty affairs, and Anna D. Wolf Chair. Every day, women come into emergency rooms across the country with injuries resulting from domestic violence.
Last summer, Campbell and other faculty members lent their domestic violence expertise in arranging the scene on the Hopkins medical campus. The purpose: the creation of an educational video to train health care providers and patient educators on how to properly respond to domestic violence.
“Thirty-seven percent of all women who seek care in hospital emergency rooms for violence-related injuries have been victims of intimate partner violence at some point in their lives, and 15 percent in the past year,” states Campbell. “Yet only five percent of abused women are correctly identified as such, and even when they are, the response that follows from providers is often inappropriate.”
For instance, an important first step is to separate the woman from her partner. “Women need to be screened in private, where they can feel safe about disclosing information,” says Campbell.
The domestic violence screening and assessment strategy used at the Johns Hopkins Hospital was developed by Campbell and colleagues served as the model in the production of the video. The cameras followed the actress throughout the day, from her initial experience in the ER with the triage nurse (played by clinical instructor Janet Selway), to the screening process with a clinical nurse (played by associate professor Phyllis Sharps), to her examination by a physician (Kim Bullock, an ER physician at Providence Hospital in Washington), to the forensic exam by a forensic clinical nurse specialist (assistant professor Daniel Sheridan). The woman eventually leaves the hospital accompanied by a social worker, who takes her to a battered women’s shelter and helps her with necessary arrangements.
“When an abused woman enters an emergency department, hospitals are given the chance to intervene and prevent future abuse,” says Campbell. “This video will help show health care providers just how to take advantage of that crucial opportunity.” For information on ordering “When Injuries Speak, Who Will Listen? A Healthcare Response to Domestic Violence,” visit www.intermedia-inc.com.
— MT
SimMan, the Lifelike Addendum
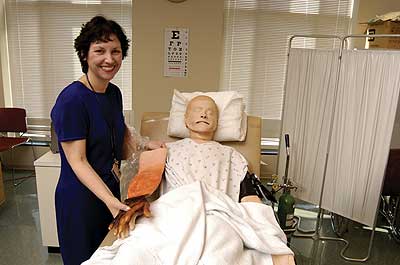
Two School of Nursing students, Marguerite Baty and Paul Schwartz, stand on either side of a patient’s bed. He lies quietly, his eyes closed. His chart says he has pneumonia. Suddenly, he begins wheezing severely.
“My chest, it’s so tight. It’s so hard to breathe,” he says, gasping. Schwartz puts an oxygen mask over his nose and mouth.
“Mr. Sims, we’re going to have to sit you up and listen to your breathing,” says Baty. She and Schwartz reach behind the patient’s back and push him up and forward.
“Don’t let me die,” replies the patient. “I have a family.”
Mr. Sims, however, can’t die. And he has no family. He is SimMan™, a computer-controlled patient simulator made by Laerdal, a Norwegian company. Costing just over $30,000, SimMan was presented as a gift to the school last fall by the classes of 1958, 1963, and 1968.
SimMan is as close to real as a manikin can get, says Diane Aschenbrenner, MS, APRN, BC, instructor of professional education programs and practice. He is blond, 5’5″ tall, and weighs 75 pounds. He talks, breathes, coughs, moans, and makes vomit sounds. Students can check his blood pressure and his pulse, listen to his heart and bowels, and insert IVs and chest tubes. Moreover, they can change his abdominal plate to make it look like a bowel is protruding, his leg to make him look like a diabetic with impaired circulation, and the skin on his hand to make him a burn victim. They can even change his genitalia.
“SimMan gives us the ability to see things we wouldn’t necessarily see in clinical placement,” says Schwartz. And students hone their skills before moving on to real patients. “We want every student to practice certain things,” says Aschenbrenner. “This enables us to do it without harming people.”
Attached to a personal computer and a compressor, SimMan is controlled by a Windows application that lets instructors preset certain medical scenarios and introduce complications with a click of the mouse.
The school also has purchased VitalSim simulator, a simpler model used for basic testing only, and is trying to raise funds for an obstetrical model and SimBaby, due out in the next year.
In the meantime, Aschenbrenner says, the school will incorporate SimMan further into the curriculum, using him to teach not only basic skills but also responses to more complicated situations such as heart attacks.
But students should not get too attached. “SimMan will never replace real patient contact. Nor will he replace real interaction with an instructor in the lab setting,” says Aschenbrenner. “We see him as an addendum.”
—KB
Asking Questions to Improve Safety
Nursing student Courtney Edwards has spent a good part of her senior year in the Johns Hopkins Hospital surgery intensive care unit, examining the adverse effects that uncontrolled glucose levels can have in patients after surgery. In another part of the hospital, classmate Vanessa Makarewicz has been tracking rates of infection caused from using vascular assisted devices. Edwards, Makarewicz, and 18 other nursing students comprise the first group of Clinical Nursing Leadership Fellows. All are questioning why things are done the way they are and delving into investigations on how procedures might be changed to improve the quality or safety of patient care.
The Leadership Fellows Program in Clinical Nursing, established at the School of Nursing last spring with a grant from the Helene Fuld Health Trust, is designed to augment the school’s leadership curriculum and prepares students to become leaders by pairing them with mentors from the clinical setting who are part of an interdisciplinary team looking at a quality or safety problem. The three-year program names 20 fellows each fall and spring semester. Fellows learn to think critically about clinical quality patient care and to take the lead within their teams to study and solve the problems.
Edwards describes the experience as a beneficial adjunct to the school’s leadership course, and says, “I look forward to presenting my findings and assisting in improving the protocol and educating the nurses.”
Adds Makarewicz, “Nursing is becoming more and more evidence-based practice, so the skills that I am learning are going to be essential out in the work force.”
Joining Edwards and Makarewicz as spring 2004 semester fellows were Michelle Berardi, Erin Connelly, Caroline Curtis, Jill Daniel, Tresa Dusaj, Nicholas Farrey, Megan O’Brien Gold, Stephanie Gorman, Megan Hoffmann, Kathleen Janosko, Marcy Kaloginnis, Jan Oosting Kaminsky, Heidi Kapustka, Christopher Killam, Leah Peterson, Amy Pettler, Claire Whitfield, and Lai Wong. Another group of fellows will be named later this spring for the fall 2004 semester. —MT
Magnets to Excellence
By Karen Haller, PhD, RN
Vice President of Nursing and Patient Care Services,
Johns Hopkins Hospital
It’s official: Hopkins’ Department of Nursing has earned the Magnet Recognition Award for Excellence, the only national award recognizing excellence in nursing. The American Nurses Credentialing Center (ANCC) handed down its ruling on November 17, 2003, making Hopkins the only hospital in Maryland and the 90th in the nation to receive the honor since the program’s inception in 1993.
The achievement marks the end of a rigorous bid for Magnet status, beginning in April with a 1,700-page documentation of Hopkins’ best nursing practices and ending with a four-day site visit in September, when three ANCC appraisers combed through the Hospital.
One person questioned by the appraisers was Phyllis Zolotorow, the mother of a long-time patient. “People don’t realize how much nurses do,” she said. “They’re making an awful lot of the decisions in patient care.” Another was Louis Ringer, intake coordinator for The Salvation Army’s detoxification facility, who works with Hopkins’ intensive treatment unit nurses to transition patients into their residential treatment program. “They understand who is right for our program and weed out the men who aren’t sincere about recovery,” he said.
The appraisers weren’t looking to fault Hopkins’ application, but witness for themselves nurses’ relationships and leadership within the hospital through such themes as evidence-based practice and interdisciplinary collaboration.
The months of preparation were worth it, according to Katie Muther, a surgical nurse who helped lead the effort. “My heart just swelled when I heard top surgeons describing all we’ve contributed.” Many physicians cited examples of nurses’ involvement in decision making and research, and their leadership in protocol development, to the appraisers. “Nurses always find new and better ways of doing things,” said George Dover, chairman of Pediatrics. “The things that used to separate nursing and medicine are disappearing.”
While this award allows us to pause and take pride in our accomplishments, it is not a static event. We are committed to ensuring that Hopkins continues to meet, and set, the highest quality standards in nursing and patient care.
Milestones
As Hopkins Nursing reaches its 115th year, the school has embarked upon a yearlong “Milestone Celebration” to commemorate notable events in its rich history, including the 20th anniversary of the School of Nursing becoming a degree-granting division of the Johns Hopkins University.
1889 Johns Hopkins Hospital opens in May. Johns Hopkins Hospital Training School for Nurses opens in October.
1892 Alumnae Association is formed with 38 members.
1926 Hampton House, named for the first superintendent of the Training School, Isabel Hampton Robb, opens as a residence for nursing students.
1973 Johns Hopkins Hospital School of Nursing graduates its last class and closes.
1974-1979 Johns Hopkins University School of Health Services Nursing Education program offers BSN degree.
1984 School of Nursing opens as a degree-granting division of Johns Hopkins University.
1987 Master’s and post-doctoral fellowship programs first offered.
1990 Accelerated program begins, with students earning a BSN in 13 months.
1992 From Baltimore to the world: Wald Community Nursing Center established to serve Baltimore’s uninsured; Peace Corps Fellows program developed.
1993 Doctoral program first offered.
1994 Center for Nursing Research established to support faculty research on ways to promote health and improve delivery of health services.
1995 Institute for Johns Hopkins Nursing established, linking education and practice.1998 Anne M. Pinkard building, the first dedicated to the education of Hopkins nurses, opens.

And the pulse goes on
In the 21st century, the School of Nursing continues to strengthen international ties, expand community health sites and programs, conduct vital health care research, and educate leaders for nursing’s future.